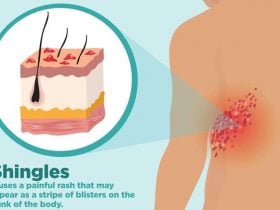
Scleroderma is a high-risk systemic autoimmune disease. [1] In this case, we are talking about a disease of the connective tissue. Small vessels, capillaries are affected by the body’s own immune cells, as a result of which metabolic processes in tissues are significantly impaired. [2] The skin, as well as the subcutaneous tissue, are strongly compacted as if they become homogeneous, similar to continuous scar tissue. The disease progresses, seizes joints, internal organs and as a result, can lead to the death of the patient.
Most often, women get sick with scleroderma, and with age, the risks of such a pathology increase.
What Symptoms Does the Disease Produce?
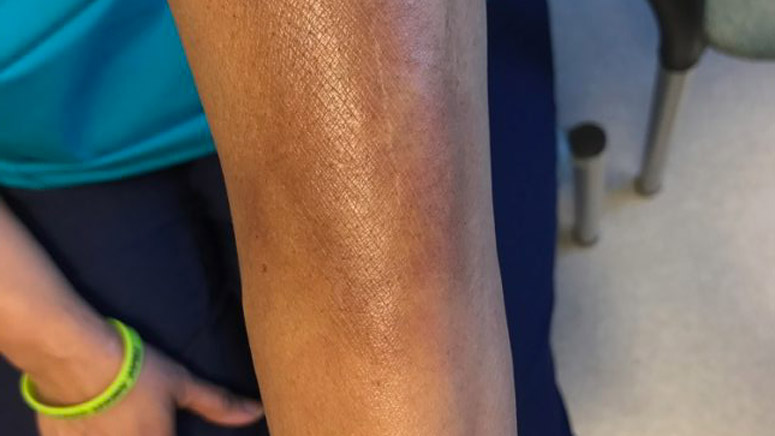
Scleroderma affects multiple organs, with the most characteristic of being skin involvement.
Skin Changes
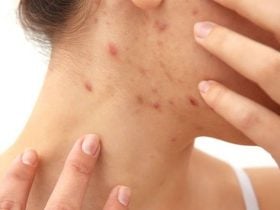
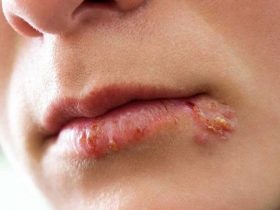
It is usually affected in all patients who have scleroderma, although there is a rare form of the disease called systemic sclerosis without scleroderma in which the skin is not affected. Scleroderma is characterized by skin changes, first in the form of swelling, and then in the form of thinning and thickening. The skin looks tight, shiny (waxed), and darker than healthy areas and there is itching that may be troubling. In some cases, changes are limited to the skin of the fingers, less often the feet (sclerodactyly i.e. thickening of the skin of fingers or toes). Sclerodactyly affects both hands symmetrically and may be accompanied by itching and tingling.
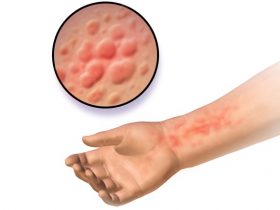
Over time, changes in skin color (darker or paler) can be seen, and small veins (telangiectasia) can be seen. [3] The atrophy of the skin facilitates wounds that give rise to painful ulcers that often cannot be closed.