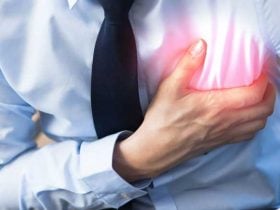
Contrary to its name, cardiac asthma is not a form of asthma. It describes breathing issues brought on by the accumulation of fluid in the lungs as a result of any heart issues including heart failure.
A correct diagnosis of cardiac asthma is essential since it may be fatal. Due to the similarities in the symptoms, it may be mistakenly diagnosed as asthma. Coughing, wheezing, and shortness of breath can occur in people with either illness.
Keep retro’s article to learn everything you need to know about cardiac asthma, including its symptoms, causes, and treatments.
Cardiac asthma: what is it?

A group of asthma-like respiratory symptoms known as cardiac asthma are brought on by congestive heart failure. In medical literature, Dr. James Hope first used the term “cardiac asthma” in 1833.
Coughing, breathing difficulties, and shortness of breath are common signs of cardiac asthma brought on by pulmonary congestion. This is an accumulation of fluid in your lungs that makes it difficult for you to oxygenate your blood.
There are four chambers in your heart: the right atrium, left atrium, and right ventricle.
When a person has congestive heart failure, their left ventricle can’t pump blood out correctly or has high pressure. This interruption of blood flow causes the blood pressure in the blood arteries in the lungs to rise, which results in fluid leaks and buildup.