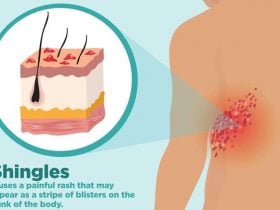
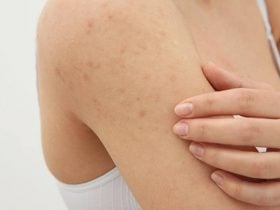
Shingles [1] is a type of viral infection caused by a broad group of viruses known as herpes virus and belongs to the same type of chicken pox infection class as the causative organism with the varicella zoster virus. Typically, in the neural tissue, someone that has been infected with chicken pox [2] would have an inactive form and it will reactivate itself like shingles for years down the road.
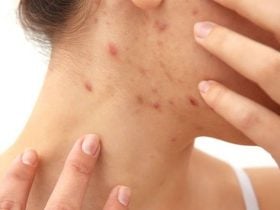
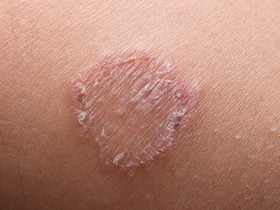
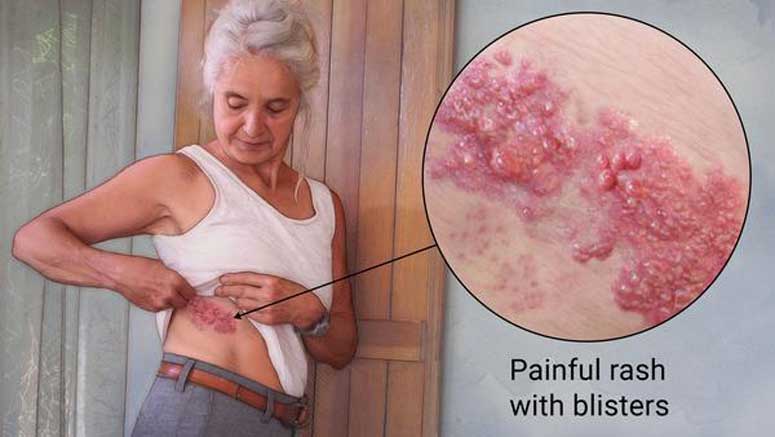
Shingles infection cause a painful rash, and can occur anywhere in the body but the most frequent site of occurrence is the trunk appearing as a single stripe of blisters. Symptoms of shingles infection include: pain, itching, crusting and blisters, fever and fatigue. Though not life-threatening, shingles can be very painful when it occurs. When treating shingles, it is best to treat them as soon as possible in order to prevent complications that could occur from delayed care. Postherpetic neuralgia is the most serious complication of shingles, which causes the condition to linger even after the infection has healed.
General Principles of Shingles Treatments
First of all [3], the administration of drugs of direct antiherpetic action (based on acyclovir) in high dosages is indicated. It reduces the severity and duration of the infectious and post-infectious (pain syndrome) process. You need to start this as early as possible – no later than seven days from the onset of the illness and three days from the onset of the rash. When the drugs are used at a later date, their effectiveness is sharply reduced, since the virus has already reached its peak of development and has caused a cascade of immunoneuropathological reactions. The use of local remedies [4] for herpes – ointments and creams – has a weak therapeutic effect. For a drying, local antiseptic effect, any local antiseptic of this kind is used – zinc talkers, brilliant green solutions. With extensive lesions, accompanied by a pronounced inflammatory reaction, anti-inflammatory drugs, glucocorticosteroids and antiallergic drugs are used. With severe pain (ganglioneuritis), standard analgesic drugs (NSAIDs) are ineffective, therefore, preference should be given to centrally acting anticonvulsants and antidepressants. Physical therapy relieves pain. Taking vitamins, dietary supplements, etc. does not have any obvious value. With uncomplicated and localized forms of the disease, the prognosis is favorable. With the development of ganglioneuritic pain, the quality of life can significantly decrease for a sufficiently long period (up to a year), and with meningoencephalitic and disseminated forms – for an even more serious period, fatal outcomes are frequent. Disease prevention in the outbreak is not carried out. After the patient’s stay in the ward for disinfection, it is enough to ventilate the room (with disseminated forms).